Our Revenue Cycle Process From Start To Finish
We manage your complete billing cycle accurately and efficiently to ensure timely payments and financial stability.
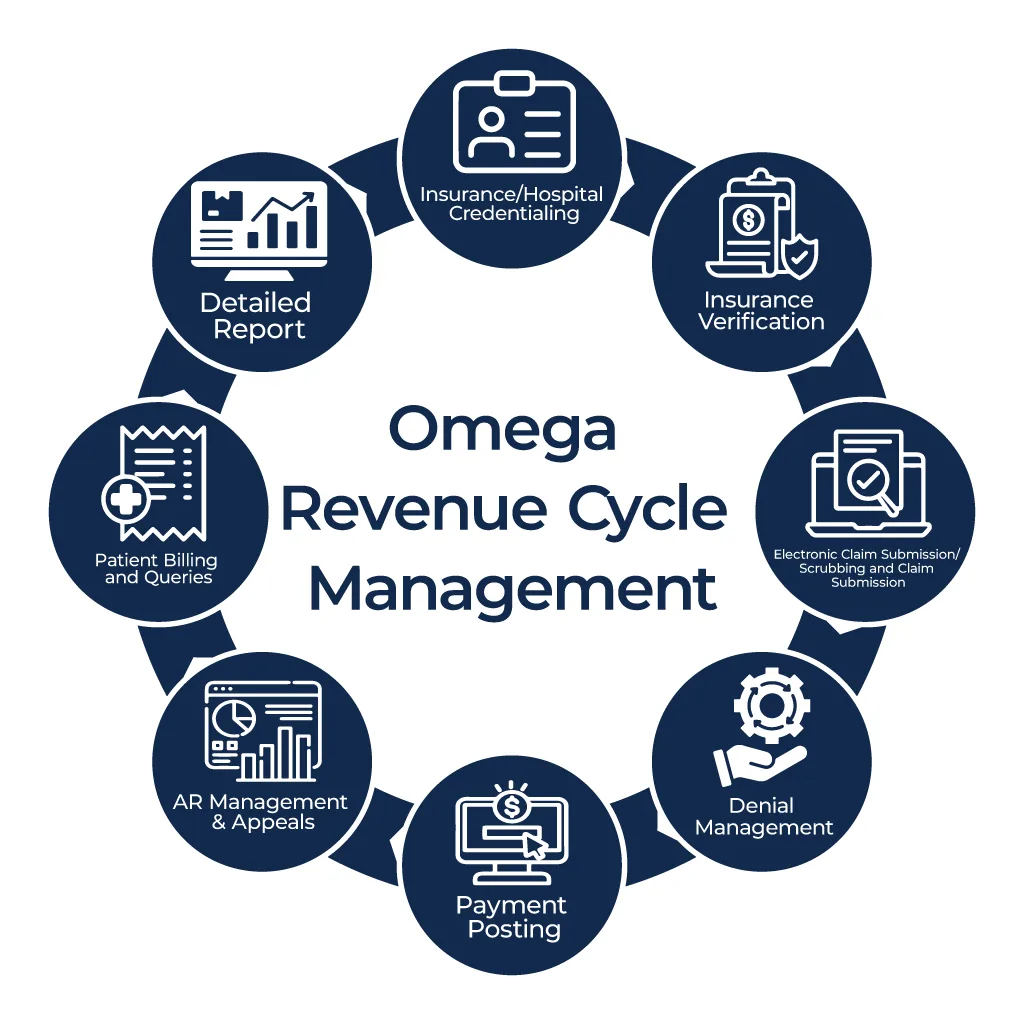
Keep your billing process accurate, secure, and fast with Omega RCM Solutions services to boost your practices revenue and profitability.
First Pass Clean Claims Rate
Collection Ratios
Reduction in A/R
Revenue Increase
We manage your complete billing cycle accurately and efficiently to ensure timely payments and financial stability.

Our team of skilled professionals is committed to providing personalized, compassionate service with a strong focus on quality, efficiency, and client satisfaction.

Omega RCM Solutions uses 25+ years of expertise and a proven three-tier approach to boost your practice's revenue while reducing costs.

We handle claims processing and staff support, delivering quality medical billing services at competitive rates with a client-first approach.

Our transparent revenue cycle management provides actionable insights and leverage opportunities to accelerate your practice's growth.









We maintain industry-leading standards through recognized certifications and affiliations.






At Omega RCM Solutions, we simplify your experience with clear answers about our services, billing, insurance claims, and provider support.
Omega RCM Solutions offers comprehensive, end-to-end billing solutions, including credentialing, accurate coding (CPT & ICD-10), clean claim submissions, denial management, and detailed performance reporting. We also manage your complete billing cycle, ensuring timely payments and a steady revenue flow. Additionally, our services include benefits verification and eligibility checks, allowing you to confirm patient coverage and streamline the claims process for improved accuracy and reduced denials.
By ensuring precise coding, prompt claim submissions, and efficient denial resolution, we maximize reimbursement and reduce delays. Our customized strategies are designed to enhance financial performance and minimize revenue leakage.
Yes! We handle the entire credentialing process, ensuring providers are properly verified and enrolled with payers to avoid delays in claims processing and reimbursement.
We proactively identify, appeal, and resolve denied claims efficiently. Our team investigates the root cause of denials and implements corrective actions to prevent future occurrences and recover lost revenue.
Absolutely. We provide detailed, easy-to-understand performance reports that help track revenue trends, patient volume, claim status, and overall growth. These insights allow you to make informed business decisions.
Yes. At Omega RCM Solutions, we understand every practice is unique. We work closely with each client to create customized solutions that align with their operational and financial goals.